What is a breast reduction?
Breast reduction surgery (or reduction mammaplasty) is designed to decrease the size and weight of large, heavy breasts.
Who is a candidate for this surgery?
Women who have neck and back pain or experience grooving at the shoulders from the weight of their breasts may benefit from reduction. Women who develop frequent skin infections under their breasts, especially during the summer, may also experience relief.
How is the surgery done?
The procedure is performed in a hospital under general anesthesia and takes three to five hours. A keyhole shaped incision is made in the skin above the nipple/areolar complex (the areola is the pigmented skin surrounding the nipple). The complex is left on a mound of breast tissue that serves as the “new”, smaller breast and the excess breast tissue and skin on both sides of the complex are removed. The skin that was originally above the nipple is moved down (surrounding the nipple and covering the remaining breast mound) and is closed with stitches. This results in a smaller breast with the nipple in a higher position. The surgery leaves a scar around the nipple/areolar complex, from the lower edge of the complex to the fold under the breast, and in the fold under the breast. The scar located within the fold is kept as short as possible and should be concealed by most clothing (eg. bras, bathing suits). Most patients go home later the same day.
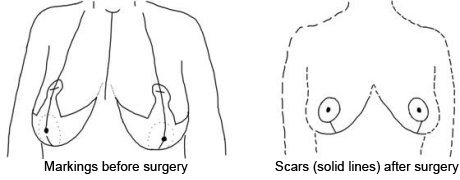
What are the possible risks and complications of this surgery?
In general, this is a very safe procedure but certain complications can occur. Because the nipple/areolar complex is being isolated from some of its original blood supply, it may lose some of its sensation or pigmentation. In rare instances, all or part of the nipple/areolar complex may die. In cases where the breasts are exceptionally large, or if the complex does not appear to have a sufficient blood supply during the operation, the complex is removed completely during the operation and sewn back on in its new position like a skin graft. In these cases the nipple looks the same but does not respond to temperature, touch or sexual arousal. Because the skin is being “rearranged”, it is also at some risk. Some of the skin, especially along the incisions, may die. This is almost certain to happen in women who smoke. For this reason, smokers MUST STOP SMOKING FOR AT LEAST TWO MONTHS BEFORE SURGERY AND ONE MONTH AFTER SURGERY. The breasts may not have exactly the same shape and size (they rarely do before surgery), although in most cases this is not noticeable in clothing. Scars are expected as described above, but they are often fine lines that fade with time (they never completely disappear). Some women may form wide or thick, raised scars which are called keloids. This is seen more commonly in people with dark skin. Some women develop scars that are red or darker than the surrounding skin. The ability to breast feed may be lost – this is entirely unpredictable. If the ability to breast feed is important to you, it is advisable to delay surgery until after having your family.
Might I need a blood transfusion during surgery?
Breast reduction can result in significant blood loss, especially in very large breasts or very young women. Transfusions are rarely necessary, but donation of a unit of your own blood prior to surgery is possible if this is a significant concern to you (donation is generally not covered by insurance plans).
What can I expect after surgery?
You will be placed into a sports bra in the operating room and will wear it continuously for the first two weeks. Small, soft drain tubes are placed in the breast to allow any fluid or blood to drain and are removed in the office in three to four days (the removal is no more painful than having stitches taken out). Post-operative pain is controlled with prescription pain medication, and after the first few days ibuprofen-type drugs work well.
You will be asked to avoid heavy lifting, pulling or pushing for the first two weeks. Walking, swimming and “non-bouncy” activities can be resumed within two to three weeks. Running, jogging and aerobics should be avoided for the first three months.
When can I go back to work?
Most patients who do not perform strenuous physical tasks at work may return at the end of the second week. Almost all patients are able to return after four weeks.
What will I look like after surgery?
Immediately after surgery your breasts will be swollen, quite high on your chest, and cone-shaped. The nipples may also appear to be too low. In the first three months the shape changes significantly. The swelling decreases and gravity causes the breast to drop to a more natural position and take on a more natural teardrop shape. The nipple will also rise to a more appropriate position. After six months the shape is usually stable. The scars will soften and fade over the first year (up to two years in some patients).
What size will I be after surgery?
I will ask for your ideal size and work toward that goal; however some limitations do exist. The base (width) of the breast cannot be changed significantly and a certain volume of tissue must be left in place to avoid a flat, masculine appearing breast, as well as to supply blood to the nipple/areolar complex.
Can my breasts “grow back” after surgery?
The surgery will remove some, but not all, breast tissue. Fluctuations in your weight as well as pregnancy will still affect the remaining breast tissue, so that increases (or decreases) in size proportional to overall changes in body weight are certainly possible. Spontaneous re-growth of breast tissue after surgery is rare except in very young patients.
Will my insurance cover this surgery?
Insurance coverage for breast reduction surgery MAY be available. Some insurance plans specifically exclude this procedure (“Reduction Mammaplasty” would be listed on the “Exclusions” page of your policy.) If not specifically excluded, the procedure maybe covered if the insurance company’s criteria are met. These vary by company and plan, however may include the following:
1. You should not be substantially over the ideal weight for your height as documented at your doctor’s office.
2. Your surgeon must be able to remove a certain weight of tissue from each breast
3. Non-surgical measures (professionally fitted bras, physical therapy, etc.) must be tried before surgery.
This document was prepared as a general reference, covering many frequently asked questions about breast reduction surgery. While I hope you find it informative, it is by no means complete. Please make a list of any additional questions you may have; you are encouraged to ask them during your consultation.